
Signaling a high-water mark in efforts to fight animal abuse, President Donald Trump today signed a law making intentional cruelty to animals a federal felony. While the Preventing Animal Cruelty and Torture Act does not specify a role or responsibilities for veterinarians in combating cruelty, an increasing number of jurisdictions do, reflecting an evolution in attitudes about animal abuse that is changing expectations of veterinarians.
The understanding that animal abuse often occurs in tandem with or as a precursor to crimes against people, especially domestic violence and child abuse, has led to anti-cruelty laws in every state, and to increasing fines and penalties for offenders. In recognition of the link between crimes against animals and crimes against people, the FBI began in 2016 to track instances of animal cruelty in its national incident database, along with arson, burglary, kidnapping and homicide.
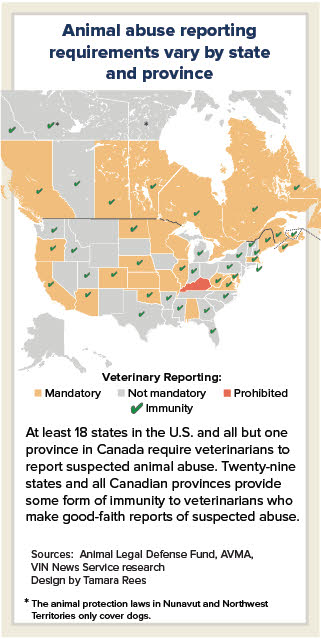
As part of the effort to curb animal abuse, 18 states require veterinarians to report signs of animal cruelty to law enforcement or other government agencies, according to information compiled by the American Veterinary Medical Association. Mandatory reporting for veterinarians is required in all of Canada's provinces except Alberta.
"Often veterinarians are the only human witnesses to the effects of animal cruelty, so it is crucial that they are empowered to report and receive civil immunity for reporting in good faith," said Kathleen Wood, a staff attorney with the Animal Legal Defense Fund, which advocates for mandatory veterinary reporting statutes.
A majority of veterinarians who responded to a survey in 2015 indicated support for the trend. Led by a researcher at Colorado State University College of Veterinary Medicine and Biomedical Sciences, the survey polled members of the Veterinary Information Network, an online community for the profession and parent of the VIN News Service. Of 1,209 respondents, 66% supported mandatory reporting laws.
However, some veterinarians have concerns. In surveys, online message boards and conversations with VIN News, some practitioners say they don't always know how to spot abuse or best practices for reporting, and they are worried about everything from violating the veterinarian-client-patient relationship to the possibility of retribution by angry clients.
Support for concept meets concern about execution
The most recent states to require veterinarians to report signs of cruelty are Massachusetts, in 2014, and Maryland, in 2018. When Massachusetts made reporting mandatory, some veterinarians told VIN News they worried that the requirement might prevent people from seeking medical care for their pets, even in cases of accidental injury.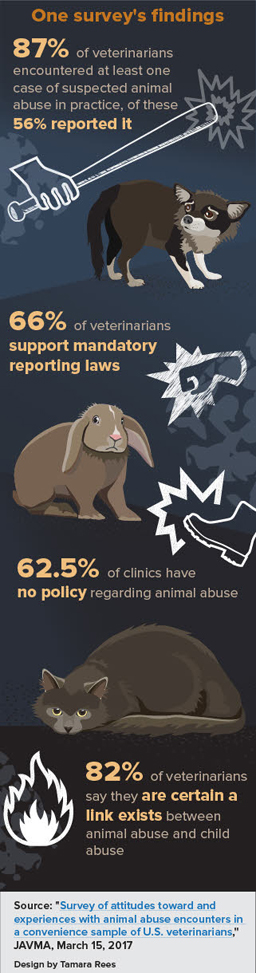
Others writing on a VIN message board voiced concern that aggrieved clients might blast veterinarians on social media or file retaliatory complaints with veterinary boards. Some expressed fear of physical harm by people who enjoy making animals fight and/or are capable of seriously hurting animals. Would authorities protect those who report? veterinarians asked.
"I doubt even if they did offer some form of protection that it would work to protect the veterinarians from future retribution," wrote Dr. Frank Marchell, who has a small animal practice in Maine. "We might assume that individuals abusing animals may hold a similar set of values for people."
Dr. Don Woodman, who has a companion animal practice in Florida, voiced concern when Massachusetts passed its reporting requirement and continues to believe that while well-intentioned, such mandatory reporting laws are not thought through.
"I one hundred percent believe veterinarians should be empowered to report suspected abuse," Woodman said in a recent email to VIN News. "BUT ... this would in my mind include shield laws protecting veterinarians from retaliation by clients, the development and dissemination of clear diagnostic criteria, and the creation of robust investigatory infrastructures BEFORE veterinarians are told that they are REQUIRED to report suspected abuse."
Woodman became interested in the topic more than a decade ago when he was trying to get the Florida Veterinary Medical Association to lobby for a law that would give explicit permission and protection to Florida veterinarians who reported abuse. He wasn't successful at the time, but he noted that a provision stipulating that veterinarians "may" report abuse was adopted in Florida earlier this year. These regulations can act as a shield against charges of violating confidentiality.
Woodman cites the example of physicians, who are required to report signs of abuse. He said that human medicine began looking at the issue in earnest in the mid-20th century. "Diagnostic criteria for abuse were developed and then practitioners were trained: 'When you see this constellation of symptoms, abuse should be on your differential list.' Then, a system of reporting and investigation infrastructure was put in place."
Without these steps, Woodman said, "I think things will be a mess. Imagine if states started requiring veterinarians to report a disease, but veterinarians were never taught about the disease and what symptoms should make one suspect the disease. … Some vets would ignore the mandate, and other vets would overreport."
Researchers studying the issue of veterinary reporting have found that veterinarians sometimes feel unprepared to identify abuse and/or know the rules and protocols for doing so.
"[T]he diagnosis of abuse, cruelty, nonaccidental injury, neglect, or maltreatment of animals is one of the most challenging subjects in clinical work," the authors of the 2015 survey wrote. "Without the appropriate education and information, veterinarians may be more likely to avoid getting involved than if they were better prepared."
Of the veterinarians who responded to the survey, 87% said they had seen at least one case of suspected abuse and 55.8% reported it. Of those who did not make a report, 36.8% said it was because they were unsure it was abuse. Other leading reasons were:
- thinking it better to educate the client than report the abuse (17.8%)
- thinking it was accidental and not intentional (9.9%)
- being unsure of the process for reporting (9%)
Dr. Lila Miller, who retired this year as vice president of shelter medicine at the American Society for the Prevention of Cruelty to Animals, believes mandatory reporting can help veterinarians. In a presentation on the veterinarian's role in handling animal abuse, she explained that it can be difficult when clients try to negotiate with a veterinarian. With mandatory reporting, Miller said: "You can just say, ‘Look, I'm sorry. I have to file a report. If you haven't done anything wrong, it's not a problem. It's just what the law requires me to do.' "
She noted that veterinarians are not investigators or prosecutors; they don't have to make the final determination.
Canada moves toward mandatory reporting
In Canada, laws in nine of 10 provinces require veterinarians to report suspected abuse. Alberta is the lone holdout but is moving in that direction. In February, the Alberta Veterinary Medical Association, which regulates the profession in that province, passed a resolution adopting mandatory reporting for veterinarians and veterinary technologists. This resolution became binding on ABVMA members on July 1 by virtue of ABVMA Council policy. The association will propose codifying this amendment in Alberta's Veterinary Profession Act General Regulation.
In addition to provinces, Canada has three territories. None require veterinarians to report suspected abuse. All provinces and territories except Nunavut explicitly offer some sort of immunity to anyone who makes a good-faith report of suspected abuse.
Despite the widespread adoption of required reporting in the country, achieving "the virtuous goal of animal protection" via mandated reporting is not without its challenges, said Dr. Gary Morgan, registrar at the Prince Edward Island Veterinary Medical Association, which regulates the profession in that province.
"People may be reluctant to reach out to a vet for treatment if afraid that they might be violating the Act and be reported by the vet," he wrote in an email to VIN News. "There is also a potential conflict of interest for the vet. For example, the patient with severe gum disease, [and a] client [who] cannot afford dentistry. The Act may interpret that as a violation, and require the vet to report the client who cannot afford the service as animal abuse."
An interagency debate in British Columbia illustrates some of the challenges of interpreting what triggers a report. The provincial government made reporting suspected abuse mandatory for veterinarians in 2011 in the Prevention of Cruelty to Animals (PCA) Act. Six years later, the College of Veterinarians of British Columbia, a regulatory body, issued a position statement on the duty to report.
"[The position statement was] intended to clarify registrants' responsibilities when it comes to the PCA Act, as there seemed to be some misunderstanding about what sorts of things would trigger that duty," CVBC Deputy Registrar Dr. Stacey Thomas wrote in an email to VIN News. Thomas recounted the history, although she was not part of the college at the time.
The statement said, in part, "Reporting a client to the BCSPCA should be reserved for circumstances where there is clear and unequivocal evidence of an animal being in distress as a direct result of the actions of the veterinarian's client."
Furthermore, the CVBC wrote: "Threatening to report or reporting on circumstantial evidence will leave veterinarians open to criticism for breaching client trust and confidentiality, eroding the veterinarian's professional reputation in addition to adversely affecting business, and most importantly, possibly preventing the animal from receiving treatment."
The province's chief veterinarian, Dr. Jane Pritchard, took issue with this guidance. Writing in the July 2017 Ministry of Agriculture newsletter, Pritchard reproved the CVBC. "The emphasis on protecting client confidentiality to defend not reporting animal cruelty seems to me to be less than professional within the context of our oath and the requirements of the PCA," she wrote.
Citing high-profile acts of extreme cruelty in British Columbia and public outrage, she continued: "The public often questions what the role of the veterinarian is in these circumstances, and if we do not speak up, take an interest, ask questions and become engaged in this area, I fear we as veterinarians will be seen as irrelevant in protecting animal welfare."
The CVBC statement was revised a few months later. It no longer makes reference to "unequivocal evidence." The updated statement says in part, "Without clear evidence of current or imminent animal distress requiring a PCAA report, it is best to proceed with reason and caution." It also calls reports potentially "devastating to all involved."
Despite reservations within the profession, momentum is on the side of mandatory reporting in Canada. The next action may come in Yukon, the country's smallest territory.
Yukon does not have a regulatory body for the dozen veterinarians who practice in the territory, and the province's Animal Protection Act has no rules relating to a veterinarians' duty to report. However, the government is in the process of updating its animal protection and control laws, according to Yukon Chief Veterinarian Dr. Mary Vanderkop.
To that end, Yukon's Animal Health Unit conducted a survey in 2018. According to results, Yukoners like the idea of requiring veterinarians to report suspected abuse of animals.
"This was supported by 82% of respondents," the survey summary said. "It was also clear that people wanted veterinarians to be protected from liability or other backlash when making these reports in good faith."
Vanderkop said the process of updating the rules could move to the legislature in 2020.