The morning that Dr. Jennifer Spurrell awoke with a sudden pain in her right wrist, she joined the ranks of veterinarians with work-related musculoskeletal injuries, although she didn't know it.
"I hadn't been doing anything out of the ordinary that week and assumed I had slept on my wrist funny and it should go away," Spurrell, a mixed animal practitioner in Ontario, recounted in a post on a message board of the Veterinary Information Network, an online community for the profession.
Spurrell took ibuprofen and visited her doctor. The diagnosis: de Quervain syndrome, otherwise known as tenosynovitis of the thumb abductor tendons.
"It's a mystery why it suddenly showed up, on a Saturday even! and how long it might take to resolve," Spurrell wrote.
She shared the experience hoping for advice on how to adapt palpation techniques on bovine patients, and to solicit comments from colleagues who left large animal practice due to injuries. She hoped others might speak to the struggle to balance physical and professional health.
Much to Spurrell's surprise, other practitioners soon chimed in with their experiences with the oddly named malady of the hand and wrist.
"I'll. Be. DARNED!!" wrote Dr. Margaret Hammond-Lenzer. "I am currently in the midst of post-surgical recovery for treatment of de Quervain syndrome which I'd never heard of before, but hurts like the dickens especially if it happens to be your dominant hand!!"
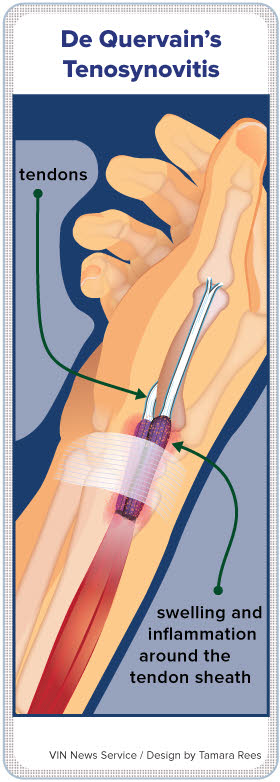
De Quervain's tenosynovitis is widely described as pain affecting the tendons on the thumb side of the wrist. It also goes under the names "nursemaid's thumb," "washerwoman's sprain," "mother's wrist," or in a more modern twist, "Blackberry thumb," "texting thumb" and "gamer's thumb."
The Occupational Safety and Health Administration describes de Quervain as "inflammation of the tendon sheath of the thumb attributed to excessive friction between the two thumb tendons and their common sheath," a condition "usually caused by twisting and forceful gripping motions with the hands."
The online discussion started by Spurrell inspired a one-question survey on VIN that asked whether veterinarians had heard of and/or been diagnosed with the syndrome.
Of 2,125 respondents, only 5 percent knew what de Quervain was and had experienced it. Another 12.5 percent said they may have been afflicted with the syndrome without knowing it by name.
According to the Mayo Clinic, risk factors for the condition include age (30 to 50), gender (female), being pregnant (likely because of hormonal changes that loosen ligaments), taking care of babies and having jobs or hobbies that involve repetitive hand and wrist motions.
According to OSHA, workers typically affected are butchers, housekeepers, packers, seamstresses and cutters.
A study by Dr. Sara White, a spay/neuter veterinarian and ergonomics researcher, suggests that de Quervain syndrome is one of a handful of painful musculoskeletal disorders to which veterinarians, too, may be prone.
White looked at the prevalence of and risk factors for musculoskeletal pain among spay-and-neuter veterinarians.
The study, published in 2012 in the journal Animals, found that pain increased with the number of hours per week spent in surgery and, separately, with decreased job satisfaction. The bulk of hand pain occurred in the right wrist. Most body pain was experienced in the neck, shoulders and lower back.
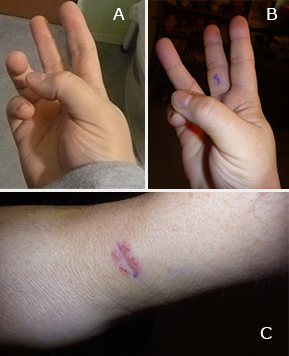
Photos of Dr. Margaret Hammond-Lenzer’s hand show her range of motion before and after surgery, and the resulting scar. In her words:
A. Before operation: "That was as far across the palm that I could flex my thumb. I couldn’t touch the tip of my pinky finger or my fourth finger with the tip of my thumb, nor could I fully extend my fourth finger with my thumb folded in."
B. One week post-op: "Range of motion in my fingers is fully restored, and even after surgery and a week in a cast, that motion was completely non-painful."
C. Post-op scar: "The leetle teeny tiny incision over the medial aspect of the carpus. Maybe 1 cm long, two sutures to close."
An association between de Quervain and veterinary work is not new. A survey of swine veterinarians by researchers examining occupational hazards also identified the syndrome as one of several potential work-related injuries. Survey findings were reported in Swine Health and Protection in 1996.
While there doesn't appear to be hard data to show veterinarians are at greater risk than people in other professions for de Quervain, White said, "Increasingly our demographics may put us at [greater] risk to the extent that it is a pregnant-, postpartum-, or middle-aged-woman risk. Also we do have a pretty physical job. And a lot of it is detailed physical stuff — dentistry, surgery, computer work — uses a lot of tendons and ligaments in our hands."
To White, these conditions are part of an overall risk of work-related injury for veterinarians. "We are not trained specifically at any point in our veterinary training how to keep our bodies safe," she said. "It's often not until we run into trouble that we have to backtrack and figure out how to fix it."
Dr. Ellie Milnes shares White's concerns about veterinarians' ignorance when it comes to ergonomics. Responding to Spurrell's message board post, Milnes, a veterinarian in Ontario, related that she once worked for a large dairy where veterinarians developed de Quervain and other repetitive strain injuries during pregnancy-testing season.
"We were losing so many vets with injuries every year that the clinic paid for all of us to have a pre-season session with a physiotherapist to identify any of our individual 'weak spots' and recommend exercises to improve our hand/arm strength," she wrote. "The physio also came out on farm with us and filmed our individual palpation techniques, then she analyzed the video with us and identified ways we could improve our technique to reduce the risk of injury. Is this something your clinic would consider implementing?"
Milnes described having a long-lasting tendon injury that cleared up after she changed her palpation technique on the advice of the physiotherapist.
She acknowledged a tendency among veterinarians "to try to tough it out, but you need to remember that keeping yourself fit and avoiding injury is better for the clinic in the long run."
In an interview by email, Milnes said, "If you are a dairy cattle vet doing hundreds of manual rectal examinations (pregnancy checks) every week, then RSI is just a part of life, so we either tough it out or switch our career path if it gets too bad."
State of mind can play a role in work-related injury, as well.
One of the strongest links in White's study was between musculoskeletal pain and job dissatisfaction. This finding is common throughout the ergonomics literature, White said. "Usually job satisfaction studies don't talk about pain, but a lot of pain studies talk about job satisfaction."
She found job stress and dissatisfaction correlated not only to the expected stress-related areas such as neck and shoulders but also strongly to pain in the hand and wrist. While White stressed that the causal relationship between musculoskeletal pain and job stress is unknown, she said, "We can hypothesize that it is probably feedback loop. Increasing satisfaction and decreasing stress can and should decrease pain."
She suspects stressed individuals change the way they use their entire bodies, working "faster or harder, less likely to take micropauses at work [to] release muscle tension."
"Also," she said, with stress, "your perception of your physical experience can change" causing an unhappy individual to focus more on unpleasant sensations such as pain. She pointed out that people's sense of control over their work situation can alter perceptions as well.
This combination of factors can lead to more fatigue, White said, regardless of the length of the work day.
Combating work-related pain does not require making major changes, White said. Instead, subtle shifts in work habits, such as taking brief pauses during activities such as surgery, can make a difference, she said. "Twenty seconds of stretching every 20 minutes can make it less painful."
Like Milnes' physiotherapist, White suggested that videotaping surgery and other procedures could provide insights into a practitioner's habitual movements. She also recommended reviewing non-work activities such as hobbies and everyday communications.
"You might be getting symptoms from surgery or instrument-handling, but also from texting and using track pad on a laptop, since both are using the thumb in a similar way," she said. "Sometimes changing something in the rest of life makes a big difference in how well the body can handle veterinary life."
Three months later, Spurrell's de Quervain has yet to fully resolve.
"I did some acupuncture," she reported. "It helped a lot. I have an appointment with the hand specialist in April. It's been a bit frustrating because I'll rest it and it'll feel better, and then I'll torque it and it'll hurt again."
Spurrell remains in mixed animal practice but is limited in her livestock practice due to the injury.
Her frustration with the slow progress is palpable. "It's still a challenge to balance what I need to recover versus what the clinic needs to function," she said. "You feel guilty making other people do calls you're normally able to do. It's a frustrating recovery, for sure."
Veterinarians may be their own worst enemies when it comes to developing musculoskeletal injuries and healing from them, White observed. "We are trying to have a stress-free and fear-free practice for patients, but we haven't quite gotten that for ourselves yet," she said.