Dog on vent
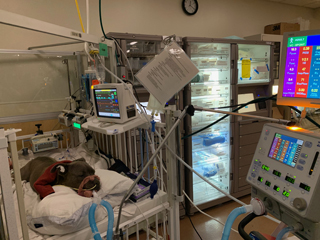
Photo courtesy of Dr. Kristen Zersen
The veterinary hospital at Colorado State University loaned ventilators, such as the one pictured, to the University of Colorado's human hospital system earlier this year to help treat COVID-19 patients. The dog in the photo is Rusko, who recovered with the help of a ventilator after nearly drowning in a lake.
Early in the COVID-19 pandemic, some hospitals in the U.S. were overwhelmed by the number of patients in respiratory distress. In especially hard-hit areas such as New York City, there weren't enough ventilators to meet demand. Veterinary hospitals helped close the supply gap by loaning out their breathing machines, which are the same as those used in human hospitals. It was a bright spot in a dark time.
The return of many of those ventilators is another bit of good news, signaling the squeeze on hospital resources has eased, at least for the moment.
While infection rates are stable in many parts of the country and still below midsummer levels, numbers of new cases are climbing in the Upper Midwest and Mountain West. Health experts warn that infections could swell during fall and winter, putting strain on some hospitals, according to a recent CNN report. Yesterday, Wisconsin opened a field hospital at the state fairgrounds about 15 minutes from downtown Milwaukee to deal with a surge in the region.
The experience of one effort to facilitate widespread sharing of veterinary ventilators has shown that the loans made a difference for human patients and that they can be counted on again if needed.
The American College of Veterinary Emergency and Critical Care spearheaded the effort in March to create a nationwide inventory of ventilators available for COVID-19 patients. No entity in the U.S. tracks available veterinary equipment for this purpose. In contrast, the United Kingdom's National Health Service called on veterinary professionals to compile a comprehensive list of veterinary ventilators early in the pandemic.
Dr. Beth Davidow, ACVECC president-elect, said the group used simple, free technology — Google forms and a spreadsheet — to compile a list of 214 veterinary schools and specialty and emergency hospitals willing to loan needed equipment. The list was shared with the Society of Critical Care Medicine, the American Medical Association and individual hospitals.
In August, ACVECC surveyed facilities listed in the inventory to see how many loaned equipment and what lessons were learned.
More than 40 life-support ventilators were sent to human hospitals, according to the survey. The total number of loaned machines is higher because some hospitals made donations without listing their inventory in the database, including several Mars Inc. facilities.
The company, which owns more than 2,000 BluePearl, Banfield and VCA hospitals and clinics in North America, donated 13 ventilators, according to an April 17 press release. Eight of these, along with 1,200 N95 masks, went to New York-Presbyterian Hospital.
Among those in ACVECC's inventory, 27 facilities reported that they had provided ventilators. Of these, 22 donations were based on existing relationships, such as a veterinary teaching hospital sharing equipment with the university's human medical facility. The majority of those that shared ventilators reported that they were deployed by the human hospitals. In one case, Davidow said, a ventilator was used for five people, four of whom survived and were discharged.
The donations really made a difference in the Northeast corridor, Davidow said. In March and April, parts of New York, Connecticut and New Jersey were a world hotspot for the virus.
Dr. Tim Hackett, associate dean of the Veterinary Health System at Colorado State University College of Veterinary Medicine and Biomedical Sciences in Fort Collins, talked to the VIN News Service in March, as he was packing up a ventilator bound for UCHealth Poudre Valley Hospital. The donation allowed Poudre Valley to send another ventilator to UCHealth Greeley Hospital, where it was needed in response to an April outbreak at a meatpacking plant. A second CSU veterinary ventilator went to a hub hospital to be deployed as needed.
In addition, the veterinary school loaned out high-flow oxygen units and 30 anesthetic ventilator systems. Most everything was returned in May. The final ventilator came back about three weeks ago, Hackett said. He reported the equipment was returned clean and well-maintained. "Everything looked as good or better than when it went off," he said.
While the ventilators were out, Hackett said no animal in need went without some form of ventilation. The hospital held onto older mechanical circuits and provided ventilation using methods practiced before they purchased their more modern equipment.
For Hackett, one of the big lessons of the pandemic was the importance of advanced planning. Colorado had a robust pandemic preparedness plan, created in 2009 in response to H1N1. That novel influenza virus was detected first in the U.S. and spread across the country and the world, killing more than 280,000 in the first year.
"That they had gone through the exercise was great," Hackett said. "We had a template." However, by 2020, many of the details in the plan were obsolete. "Protocols and contacts need to be kept up to date," he said. "Otherwise, you spend the first day trying to figure out who the new people are."
Providing support to human health care partners was another change from the norm. Typically, university veterinary hospitals call on human hospital partners for equipment or a drug it doesn't have on hand.
"We aren't usually in the position of having something they need," Hackett said. It felt good to return the favor.
The August survey also brought a few lessons and suggestions about loaning equipment to the surface.
Dr. Deborah Silverstein, a critical care specialist and professor at the University of Pennsylvania School of Veterinary Medicine, described a few key takeaways in an email to VIN News. The teaching hospital sent two ventilators, including a brand new one, to Penn Medicine, the university's human health system. Both have been returned.
Silverstein said there were fewer training opportunities for residents while the machines were out. She suggested preparing other materials for residents, such as case examples and lectures. Her team purchased a lung simulator but found it required a lot of learning and practice to use effectively.
In addition, she warned, "There will be normal wear and tear on machines, so expect this if the human hospital is busy."
She also recommended prior to transport removing all extraneous parts, such as poles for fluids, tube clamps, humidifiers and oxygen regulators. "Take pictures of machines in case they come back outfitted differently," she said, or items get lost along the way.
The hospital and the ventilator manufacturer were accommodating about replacing missing parts, she added.
For Davidow, the biggest lesson may have been simply proof of concept. "Knowing we can do it is useful," she said.