
!This story has an important update
CAPS 288

Photo by Gemina Garland-Lewis
Dr. Katie Kuehl prepares to take samples from a dog in a Seattle home where at least one resident tested positive for COVID-19. Kuehl is one of two veterinarians collecting nasal, oral and rectal swabs for a study on SARS-CoV-2 in pets.
A sick German shepherd in Long Island, New York, that tested positive for SARS-CoV-2 early this month joined a short list of pets known to be infected with the virus that causes COVID-19.
To date, two dogs and four cats in the U.S. have tested positive or were found to have antibodies, according to the U.S. Department of Agriculture Animal and Plant Health Inspection Service. All were from homes in which at least one person was infected.
A few more pets outside the U.S. have also tested positive: one cat in Belgium, one in Germany, one in Russia and two in France, and two dogs in Hong Kong, according to the World Organisation for Animal Health.
While COVID-19 is a zoonotic disease, meaning it originated in animals (bats being considered the likeliest possibility), it predominantly affects humans. Epidemiologists believe the isolated instances of pets becoming infected are most likely cases of human-to-animal transmission. There is no evidence of companion animals spreading the virus to people. However, there are reports of suspected transmission from mink to humans.
To better understand rare human-to-animal transmission events, researchers in the U.S. and Canada are conducting four separate regional studies, screening pets to gauge the rate of transmission, and to identify whether certain behaviors make humans more likely to infect animals in the home.
"We have many questions to answer, and we have to start with some basic ones," said Dr. J. Scott Weese, an infectious disease veterinarian who is co-leading one of the studies, at the University of Guelph's Ontario Veterinary College. "Knowing how often this virus moves from people to pets is a key first step."
So far, no positives
The four studies vary a bit in design (see sidebar). Three — in Texas, Washington state and Ontario — focus on mammalian pets in households where at least one person has tested positive for or exhibited symptoms consistent with COVID-19.
Veterinarians visit the homes of enrolled volunteers to collect from their pets some combination of nasal, rectal, oral and fur swabs, and blood samples for studies at Ontario Veterinary College, Texas A&M College of Veterinary Medicine & Biomedical Sciences, and a collaboration between the University of Washington and Washington State University.
A study at Cummings School of Veterinary Medicine at Tufts University casts a larger net taking volunteers from households whether they are COVID-19-positive or not. Dr. Jonathan Runstadler, a veterinarian and disease ecologist who heads the lab running the Tufts study, said there are benefits to the approach.
"It is clear that COVID-19 can be asymptomatic in some people and that virus can be shed prior to clinical signs in people," he wrote in an email to VIN News. "We didn’t want to exclude these scenarios from potential (and maybe more likely) scenarios for transmission."
In a new phase, Tufts will be recruiting pet owners who were recently diagnosed with COVID-19.
Ferret swab Tufts 288
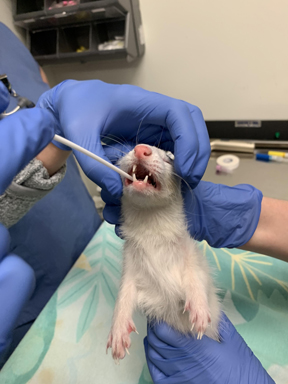
Tufts University photo
Clinical veterinary staff at Foster Hospital for Small Animals at Cummings Veterinary Medical Center at Tufts University swab a ferret's mouth to collect a sample to test for a study of SARS-CoV-2 in pets.
Unlike the other studies, Tufts includes farm animals. "Many agricultural species experience close interaction with human caretakers and, just like pets, could be infected by the virus," Runstadler said. "It’s more difficult to sample, but we’d like to get samples from these scenarios."
Farm animal samples are collected primarily from animals housed on campus or cared for by school veterinarians in the field. The team also is working with wildlife rehabilitators, zoos and aquariums to collect samples from wild animals that are in close contact with humans.
Companion animal samples — nasal and oral swabs and blood samples — are collected from animals receiving care at one of five Tufts-affiliated hospitals; and from pets whose volunteer owners submit swabs using kits provided by the study.
All four research efforts use a polymerase chain reaction (PCR) test to screen for the virus in swab samples. In the case of a positive result, researchers will try to culture the virus to sequence the viral genome.
"[W]e can compare those genomes with human sequences from their owners or the circulating human strains to provide additional evidence that the virus was transmitted from human to pet or vice versa, if those sequences are identical or sufficiently similar," Runstadler said. "However, this is not proof, as the SARS2 virus is slow to mutate (relative to influenza), and is quite similar regionally. Combined with epidemiological evidence though, it may provide insight."
So far, only the Tufts and Washington studies have test results — the more than 400 combined animals have been negative for the virus.
Runstadler concedes that PCR tests may miss some positives. "I suspect that we will find through serology [testing blood to find antibodies] that more pets are exposed than we detect from screening for virus," he said, since antibodies remain after the virus has cleared the host. "But I hope this remains restricted to rare transmission events, meaning low risk for veterinarians and low risk for our animals."
None of the studies is doing serology testing at the moment, although all intend in the future to test pets' blood for antibodies. Washington and Texas have collected blood samples from the start, and Tufts recently began collecting blood.
What behaviors make humans riskier to our pets?
CAPS photo 4 288

Photo by Gemina Garland-Lewis
Cats being generally unwilling to be poked and prodded, this study subject in Seattle is snuggled up in a towel before researchers collect samples for a study of COVID-19 in pets. The University of Washington/Washington State University study generally dispatches two veterinarians to wrangle participating cats in their homes.
While the first aim of these studies is to assess overall transmission rates from humans to pets, a second aim is to determine whether any owner behaviors increase the risk of transmission to animals. To this end, the studies ask participants to fill out surveys describing their relationships with their pets.
"We’re asking things like, ‘Do you share a bed with your cat? Do you share a bed with your dog? Do you have them with you in your kitchen when you’re eating? Do you wash your dishes together with their bowls?’ Things like that," said Dr. Julianne Meisner, a veterinarian and epidemiologist at the University of Washington. "We’re essentially treating [these behaviors] as risk factors."
Meisner expects most people will report hugging and kissing their pets, while other behaviors are likely more variable, which could make them good predictors for transmission risk.
"We anticipate bed-sharing is probably going to be a big one," she said, "because I think that’s quite different between households, especially for dogs."
One question for cats revolves around whether they are kept indoors or allowed outdoors, Meisner said. While indoor cats that presumably have more contact with humans might be more likely to be infected by their owners, she said, there is recent evidence that cats can infect one another, potentially creating a risk for outdoor cats. The study may help determine which lifestyle puts them at higher risk, Meisner said.
The Washington researchers hope that any insights will help people protect their pets if they, the owners, become ill. "If we find that cats get really, really sick, then maybe if you have COVID, you really need to pull out all the stops to get somebody else to take care of your cat," Meisner said. "But perhaps if dogs don’t really get sick, then maybe it’s not so critical [to find outside care] for dogs."
Runstadler, at Tufts, noted that the studies will need many samples to make robust judgments about the question of behavioral risk factors, but that researchers can make good use of any result they manage to get.
"[E]ven for rare cases, we’re interested in what happens to the virus when it infects a new host, so even a single positive event could be informative for us," he said.
Testing pet owners next
The Washington and Tufts studies plan to collect samples from owners whose pets test positive. This will allow researchers to do some degree of contact tracing between animals, their owners, and perhaps other people the pet has been around.
Dog swab Tufts 288
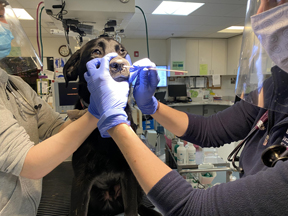
Tufts University photo
A good dog submits to a nasal swab at Foster Hospital for Small Animals at Cummings Veterinary Medical Center.
"Once we establish the risk to pets of their owners being positive, the next thing we want to ask is, what about those pets? What risk are they to humans? That’s obviously a question on many minds right now," Meisner said, noting that this phase of the research depends on identifying one or more pets positive for the COVID-19 virus, and obtaining additional funding from the National Institutes of Health. "We’re fairly confident that pets aren’t infecting humans at any appreciable rate, because if they were, I don’t think we’d have missed that signal by now," Meisner said. "But we would like to know if it happens at all."
The Ontario researchers are not taking human samples because as Weese said pet-to-human transmission would be hard to determine. "If we sampled people in the household and someone beyond the initially infected person was positive, it would be impossible to say whether that came from a person or the pet," he said. "The only way to figure out pet-to-human transmission would be to know that people are negative before exposure to the pet."
Meisner agrees this is a challenge. "Even if you do whole-genome sequencing, and there’s a perfect match, it could just be that [the human and their pet] both share the same source of infection, not that one infected the other," she acknowledged. For this reason, she said, the researchers plan to burrow deeper, by sampling close human contacts outside the household, as well. For example, if a dog tests positive and it went to a groomer during a period when it may have been infectious, they'd want to test the groomer.
"It is likely we may not be able to assess [the] direction of transmission," Runstadler at Tufts said, "but we can look at any mutation or lack thereof that may help make transmission and infection possible in a different host."
Study leaders agree that ultimately, the more information we have, the better. "We are interested in the circumstances whereby even rare transmission events occur and why," Runstadler said. "This is also a continuing epidemic, and we need to be cognizant that things might change with continued exposure to the virus."
COVID-19 research in pets
Coronavirus Epidemiological Research and Surveillance (CoVERS) study, Cummings School of Veterinary Medicine at Tufts University
Start and status: End of March; more than 400 animals tested so far; sampling to continue until human pandemic is controlled.
Eligible: Households in Connecticut, Massachusetts, New Hampshire, Rhode Island and Vermont; COVID-19 status not requested. Second phase of the study will include a cohort of pets in households with at least one resident who has tested positive for COVID-19.
Animals: Dogs, cats, ferrets, rabbits, horses, cows, pigs, mice, hamsters among others
Samples: Veterinarians collect nasal and oral swabs, and more recently blood, from pets receiving care at any one of four affiliated clinics or the Cummings Veterinary Medical Center at Tufts University, or pet owners participate from home by collecting swab samples using "swab and send" kits provided by the study.
Testing: Swabs tested using PCR (polymerase chain reaction) for SARS-CoV-2 and influenza A virus; genome sequencing conducted on positive samples. Serology testing to be added this summer.
COVID and Pets Study (CAPS), University of Washington Center for One Health Research and the Washington Animal Disease Diagnostic Laboratory at Washington State University
Start and status: Mid-April; animals (16 dogs, 7 cats) in 17 households tested so far; aiming for 100 households
Eligible: Households with at least one resident who has tested positive for COVID-19 in King and Yakima counties, Washington
Animals: Cats, dogs, ferrets, hamsters
Samples: Nasal, oral and rectal swabs and blood samples collected by veterinarians at the home
Testing: Swabs PCR-tested for SARS-CoV-2; blood banked for antibody tests. Genome sequencing conducted on positive samples, contingent on funding.
Coronavirus in pets study at Ontario Veterinary College, University of Guelph
Start and status: Late April, approximately 60 households participating; recruitment is ongoing.
Eligible: Households with at least one resident diagnosed with or exhibiting symptoms consistent with COVID-19 within two weeks of enrollment in Burlington, Guelph, Mississauga and Waterloo in Ontario, Canada
Animals: Cats, dogs, ferrets
Samples: Nasal, rectal and fur swabs, collected by veterinarians at the home
Testing: Swabs PCR-tested for SARS-CoV-2; genome sequencing conducted on positive samples
COVID-19 and pets research at Texas A&M University, College of Veterinary Medicine & Biomedical Sciences, Sarah A. Hamer Laboratory
Start and status: Mid-June; samples collected from 13 animals; aiming for 300 animals
Eligible: Households with at least one resident who has tested positive for COVID-19 in Brazos County and surrounding areas, Central Texas
Animals: Cats and dogs
Sampling: Oral, nasal, rectal and fur swabs, and blood samples, collected by research team at the home
Testing: Swabs PCR-tested for SARS-CoV-2; genome sequencing and viral propagation conducted on positive samples. Blood banked to test for neutralizing antibodies.
The Molecular and Epidemiological Study of Suspected Infection (MESSI) at Duke University’s Center for Applied Genomics and Precision Medicine is collecting nasal and throat swabs, blood and, in some cases, urine samples from people living in households where at least one resident has been diagnosed with COVID-19 in and around Durham, North Carolina. While the study is not focused specifically on companion animals, researchers are collecting oral and nasal swabs from pets in some participating homes.
Update: A dog in Georgia has tested positive for SARS-CoV-2, according to a July 1 announcement from the Georgia Department of Public Health. The dog is the second in the U.S. to test positive for the virus that causes COVID-19.