Artificial limbs for animals are slowly gaining popularity but aren't always appropriate
Pete
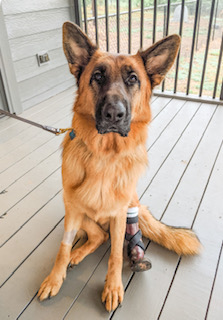
Photo by Claudia Eaton
Pete, a 2-year-old German shepherd, sports a prosthesis that he received last month. "All I want for Pete is his best life, however his best life can be," says his owner, Claudia Eaton.
Dr. Dicki Kennedy, a certified canine rehabilitation practitioner, started venturing last year into the small but slowly expanding realm of animal prosthetics. She describes her experiences so far in that world — often represented on social media by heartwarming images of cute, semi-bionic critters — as "mixed."
Kennedy initially had a reasonably good experience with a wheeled cart, ordered for a Puli named P!ink (pronounced "Pink"), who's missing one forelimb and has a deformity in the other. "P!ink is an active little dog, so she tends to tear the cart up," the South Carolina-based veterinarian said. "But when it's working, she gets around like nobody's business."
So when another client was mulling how to treat her German shepherd, Pete, Kennedy urged the client to consider a prosthesis. This time, an artificial limb was deemed appropriate because Pete was born with a deformed hindlimb.
Last September, Pete received a prosthesis that Kennedy describes as a "peg leg." Things started out promisingly: He accepted the device and his posture improved. But in the ensuing months, Pete's leg kept popping out of the device, prompting his owner, Claudia Eaton, to seek a replacement from another prosthetic company.
"He's got a ski-slope one now, and it's just awesome," Kennedy said, describing the ski-shaped boot Pete received last month. "I mean he's doing so much better …"
It still hasn't been easy going. For instance, a rock recently got stuck in the device, hurting Pete. "We don't know how the heck he got one down there, but he ended up with a bruise," Kennedy said. Fine-tuning has included sticking some Velcro on Pete's new boot to stop it from slipping about.
Kennedy's experiences are emblematic of the struggles pet owners might face when applying prosthetic devices, which long have worked well on humans, to their nonhuman friends. Some practitioners insist the rewards are worth the effort — potentially more so as advances in 3D-printing technology promise to lower manufacturing costs and help devices fit more snuggly. Veterinarians, some muse, could even make 3D-printed prosthetics in their own clinics and homes.
Among enthusiasts is Dr. Sherman Canapp, who is something of an old hand in the prosthetics business. A board-certified specialist in veterinary surgery, as well as in sports medicine and rehabilitation, he's been helping to fit prostheses, such as artificial limbs, and orthoses, such as braces, to dogs and cats for more than 15 years.
Now, Canapp applies devices to patients on a daily basis at his practice in Maryland. Most regularly, clients want orthoses — devices fitted to an injured body part for support or to help it heal. Braces, wraps and slings can be especially popular with owners who can't afford expensive surgery but want to improve their pet's quality of life.
Still, Canapp acknowledges that prosthetics and orthotics still are finding their feet, so to speak, within a veterinary community that only recently started taking the broader concept of physiotherapy seriously.
"It's been a slow boil," he said, when asked if demand for prostheses is growing. "I would say that there's been a very, very slow and gradual acceptance, mainly because it's just not taught much in veterinary school."
Cost also can be a barrier. Devices custom-made by established companies such as Bionic Pets, Animal Ortho Care, OrthoPets and K9 Orthotics and Prosthetics, can cost between $1,000 and $2,000 each. And that doesn't include any associated veterinary fees for case assessment and rehabilitation. Some animals will require a prosthesis because they were injured, say in a car accident, so their owners may already have paid thousands of dollars for surgery before the idea of a prosthesis comes to mind.
Moreover, even with the best intentions, prosthetic limbs don't always work. Animals can gnaw at devices, perhaps causing damage, or struggle to adapt to and use them properly. Prostheses can even cause animals more harm than good, should they worsen posture or wear on skin, muscle and bone.
Can three legs function as well as four?
Dr. Michael McFadden, a board-certified veterinary surgeon based in Houston, hasn't had great experiences with artificial limbs.
"I have done a few partial amputations for owners to get prosthetics and have regretted them," McFadden wrote in early 2020 on a message board of the Veterinary Information Network, an online community for the profession and parent of VIN News. "In the end, the pet suffered."
Pets requiring amputation often have the entire limb removed, since attempting to walk on a stump can cause the spine and pelvis to twist problematically. The stump itself might also become injured because the animal no longer has a paw for padding.
McFadden recalled an instance in which the owners never ended up getting a prosthesis, and their dog traumatized its stump. In other cases, animals that had been fitted with a prosthesis, he said, developed "constant sores" due to rubbing, making them reluctant to wear their device. "That leaves a stump that gets traumatized even more because they still try to use it, especially when getting up."
There also is a question of need. "We all know that pets do quite well as an amputee," McFadden said. "For most cases where a single limb is involved, going the prosthetic route is more for the owner than the pet."
McFadden's last point may chime with anyone who's ever seen a three-legged dog happily running around a park, seemingly unaware that anything's amiss.
Other practitioners, however, maintain that artificial limbs can provide long-term health and well-being benefits to animals, even if they've lost only one leg.
"If it's done right, it absolutely can improve their function and their quality of life because it's going to help with so many compensatory issues that develop over the course of their life," said Canapp, referring to the tendency for animals to put heavy pressure on their remaining limbs.
Dr. Denis Marcellin-Little, a professor at the University of California, Davis, School of Veterinary Medicine who's been fitting prostheses to animals for three decades, suggests the situation isn't black and white.
"Statements such as 'Dogs do well on three legs' or 'Dogs can't walk on three legs' are very oversimplified," he said. "Locomotion and mobility are not that simple."
Patients growing with an incomplete limb will generally develop orthopedic problems in other limbs, according to a paper Marcellin-Little co-authored, published in 2015. And size, the paper says, matters. "These problems, subjectively, are more likely to develop in larger and heavier dogs," it said.
Video by Claudia Eaton
This video of Pete mingling with his canine friends was taken on April 19, the day he received a new ski-shaped prosthesis. He previously had a peg-legged boot but his foot, deformed since birth, kept popping out.
In that vein, dogs typically are more likely than cats to receive prostheses, though felines can and do have devices fitted. Among the first was Oscar, a cat who received prostheses for both hindlimbs in 2010 after a run-in with a combine harvester. In his case, Oscar’s "intraosseous transcutaneous" devices were fixed to his bones, offering the advantage of increased stability and less infection risk, but the disadvantage of not being detachable. Birds also have received prostheses, along with a menagerie of other animals, including goats, donkeys and elephants.
"The world of exoprostheses is complex and still in its infancy," Marcellin-Little said. (Prosthetics may also be placed inside the body, in the form of artificial bones and joints, for example). "The fact that one person chooses to do something does not mean that everyone can do or should do the same thing."
To the extent that cost is a barrier, Derrick Campana, founder of the company Bionic Pets, suggests that pet owners should weigh the price of a device against the potential expense of treating compensatory-related injuries that may emerge later in life. "People think prosthetics are just for the rich, but they can be very cost-effective," he maintains.
Campana has a background in kinesiology and biomechanics and started out developing prosthetics for humans. He switched to animals in 2005. He counts Canapp as a regular client and has drawn public attention to the field with a television program called The Wizard of Paws.
Bionic Pets sells about 100 devices each month, Campana said, adding that he could sell 300 to 400 if he had more time and wanted to expand. Although he recommends the involvement of a veterinarian, Campana also sells devices direct to pet owners.
At the same time, he and Canapp say they regularly turn prospective clients away, for a host of reasons.
Contemplating a prosthesis? Consider this …
Whether a prosthesis works depends largely on which limb has been affected and how much of the limb is intact. If a patient still has an elbow or a stifle (knee), for instance, there's a much better chance they will accept the device.
"Those hinges are so important and give you much more ability to make a more functional device for the animal," Canapp said.
Pete's new boot

Photo by Claudia Eaton
Pete's new boot was manufactured by Advanced Prosthetics, a human prosthetics company that has branched into the animal realm. The titanium blade on the device has since been trimmed because it was a little long and caught on things. "It's made a huge difference and he can now move more smoothly," Eaton said.
Full-limb prostheses, although not ideal, can be functional, too. Campana has applied jacket-like devices worn on the torso, to which an artificial limb can be attached. However, these work only for forelimbs, and are recommended for "outdoor supervised use on fairly level terrain," Campana said. Indoors, it would be difficult for the animal to jump, use stairs or lie down.
If a hindlimb is amputated above the hock (ankle), Campana suggests a wheeled cart for small or older dogs that may have other orthopedic difficulties. "We’ve found young or otherwise healthy and mobile dogs don't respond well to being placed in a cart since it actually will limit their freedom of movement," he said.
Another consideration is the length of time that has passed since the animal was affected by an injury or deformity. The sooner the device is fitted, the better.
"If you don't get the artificial limb on them quickly enough, they won't accept it as easily," Canapp said. "They just don't understand: 'Why all of a sudden are you coming at me with this new device? I'm getting along fine with my other three legs. I don't need this.' "
No matter the situation, dedication by the owner is paramount, Canapp says — a point with which Eaton, Pete's owner, wholeheartedly agrees.
"The thing about having a dog with a prothesis is that it's a commitment," Eaton said. "It's constant observation: Cleaning the boot, making sure his stub remains healthy."
A 3D-printed future?
3D-printing, also known as additive manufacturing, involves making three-dimensional objects out of materials — such as plastics, resins and metals — from a digital file. 3D-printing machines can cost anywhere from a few hundred dollars to many thousands of dollars, depending on their capabilities.
The technology has myriad applications in veterinary medicine, according to Dr. Jonathan H. Wood, an assistant clinical professor and neurologist at Cornell University. Wood has a professional interest in the use of the technology, having designed, while at the University of Pennsylvania in 2017, a 3D-printed prosthetic leg for a Mealy Amazon parrot named Pete.
The printers, he said, can assist in teaching or surgery preparation by allowing practitioners to create replicas of body parts for as little as $50 each. Other applications include creating drill guides that could, say, be placed on a patient's spine to make sure screws are located correctly.
As for prosthetics, Wood is enthusiastic about 3D-printing's potential to make manufacturing not only more efficient but easier to customize.
Roxy

Photo courtesy of Bionic Pets
An artificial limb usually works better if a patient has an intact joint or joints, such as an elbow, carpus (wrist), stifle (knee) or hock (ankle). Full-limb prostheses, like the one pictured on Roxy, aren't ideal but can be functional in some circumstances — typically on forelimbs. Roxy's device has since been upgraded with a different foot.
"If a 3D-printed prothesis doesn't quite fit, you can always print another one overnight, and in the morning, you've got a new one," he said. "Or you could print three objects, all with slight variations of each other."
In the corporate space, Bionic Pets was involved in a 3D-printing joint venture with DiveDesign (which happened to manufacture P!ink's cart and Pete's initial peg leg), but the two companies recently parted ways. Campana said he found it cheaper and faster to revert to an older thermoformed-plastic technique, which involves heating plastic and pulling it over a plaster mold of a patient's stump.
Still, Campana says he might use 3D-printing again. "We're trying to work out little kinks around timing and cost," he said.
DiveDesign, meanwhile, has plowed ahead on its own, having created the company 3D Pets. DiveDesign's co-founder, Alex Tholl, remains excited by the technology's capabilities. "Not only is there a business case, the methods, results and outcomes far succeed that of the outdated thermoforming," Tholl, who has a background in industrial design, said. "Unlike thermoforming, 3D printing allows us to make the devices flexible in specific areas and rigid in others, breathable in all areas, waterproof, and more accurate with fit."
Taking a more philosophical view, Cornell's Wood said he's especially passionate about 3D printing because it could democratize manufacturing in the veterinary realm.
"It changes the balance of power where anyone with a few hundred dollars can go out and buy a printer, start sharing what looks like a good prosthesis online and invite feedback from someone else halfway around the world," he said.
For his part, Canapp is optimistic that veterinarians could one day make prosthetic devices in their own practices. He believes, though, that printers are more likely to pop up in hospitals like his own that have specialist rehabilitation therapy capabilities, as well as hospitals in universities.
Kennedy, the practitioner based in South Carolina, would consider recommending prostheses to other devoted owners, despite her trials with Pete. And she believes that if anyone can adopt 3D-printing technology, veterinarians can.
"Veterinarians, we're all kind of like cowboys," she said. "I mean it sounds terrible, but we're often like, 'Oh, you know what? I can do that. Not a problem. I'll make it myself.'
"Personally, I don't have the money to do 3D-printed prosthetics now," she added. "But yeah, we could cowboy up."