
Vaccinating horse 288

Thailand Department of Livestock Development photo
Drs. Khanitha Thitidilikrat (left) and Nithinan Nakburi vaccinate a horse in Thailand's Phetchaburi Province for African horse sickness. The disease has killed some 470 horses in the country to date.
Veterinarians are racing to contain an especially lethal disease outbreak that is threatening to devastate Thailand's horse population and jump further across international land and sea borders.
Dozens of practitioners across the Southeast Asian nation last week started administering vaccines to thousands of horses to protect them from African horse sickness (AHS). At least 470 horses have perished from the disease in recent weeks, according to Thai authorities, and there are concerns it could kill thousands more.
With a mortality rate of 70% to 95%, the insect-borne viral infection is the stuff of nightmares in global equine circles. The only vaccines currently available for AHS are of the live-attenuated variety, meaning they contain live, albeit weakened, pathogens. The vaccines are effective but not optimal because they can potentially sicken horses, especially if not administered correctly, or lead to the creation of new genetic variants of the disease.
Horses have no natural immunity to AHS. Treatment options tend to be limited to isolation, rest and palliative care. Euthanasia often is called for.
"They're dying very rapidly," Dr. Siraya Chunekamrai, a veterinarian and equine specialist on the team leading Thailand's response to the outbreak, told the VIN News Service. She pegs the horse mortality rate so far at 95%, indicating the presence of a particularly deadly strain.
Chunekamrai is coordinating and guiding more than 100 veterinarians who are responding to the disease, many of them volunteers.
"We are seeing some very acute signs, with both cardiac and pulmonary forms," she said Friday by telephone from Bangkok, having just returned that day from a disease hotspot near the Pak Chong area in the south-central part of the country, about 180 km (112 miles) away. Clinical signs have included fever, depression, conjunctivitis, swelling above eyes and lips, and dyspnea (labored breathing). Horses are dying in as few as one to three days after first displaying signs.
AHS, thought to have originated in Africa, is spread by tiny, blood-sucking midges of the genus Culicoides. AHS is listed as a notifiable viral disease by the World Organisation for Animal Health (OIE) because of its severity and risk of rapid global spread.
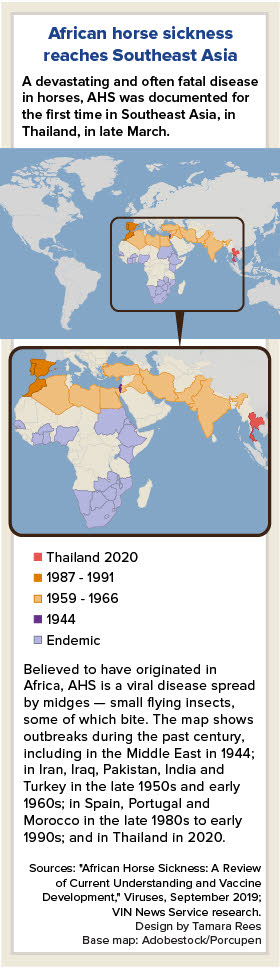 Occurrences of AHS have been mostly in African nations, including South Africa and Zimbabwe, where the disease is endemic and responsible for the deaths of multitudes of animals. In instances that it has spread more widely, the consequences have been equally devastating.
Occurrences of AHS have been mostly in African nations, including South Africa and Zimbabwe, where the disease is endemic and responsible for the deaths of multitudes of animals. In instances that it has spread more widely, the consequences have been equally devastating.
More than 300,000 equids are estimated to have died in the late 1950s and early 1960s after one of the disease's nine known serotypes, AHSV-9, spread from Africa through the Middle East and then on to India and Pakistan, according to a review paper published last September in the journal Viruses.
According to the paper, "African Horse Sickness: A Review of Current Understanding and Vaccine Development," authored by researchers at the University of Capetown, the last major outbreak outside Africa occurred around 30 years ago, when thousands of horses perished in Spain and Portugal between 1987 and 1991. That particular outbreak is thought to have originated from a zebra, with the AHSV-4 serotype, that was imported from Africa to Spain. Insects subsequently spread the disease further on the Iberian Peninsula. Zebras and African donkeys are resistant to AHS, and mules are less susceptible to the disease; ponies and European donkeys are more severely affected.
The first cases of AHS were recognized in southern Africa about 50 years after Dutch settlers introduced horses there in the mid 1600s, according to the review paper. At least 10 major outbreaks have since occurred on the African continent, including one in 1854 and 1855 that killed about 70,000 animals.
The outbreak in Thailand is the first in Southeast Asia. Samples from Thai horses analyzed at the Pirbright Institute in Woking, England, all identified the AHSV-1 serotype — marking the only time that particular serotype has ever been discovered outside of Africa. Thai authorities are investigating reports of zebras being imported recently to Thailand but no conclusions have yet been drawn about the outbreak's origins. The movement of horses throughout the country has been banned, as has the export and import of equids to and from Thailand.
Australia, China among countries on the alert
Officials from the United Kingdom down to Australia are growing alarmed about the prospect of an outbreak savaging their multibillion dollar equine industries.
AHS-free countries are believed to be increasingly at risk due to the northward migration of the midge vector as a result of climate change, according to authors of the review paper.
"Such an AHS outbreak in Europe would have significant economic and emotional consequences for horse owners on the continent, indicating the pressing need to develop new, safe, efficacious and cost-effective vaccines which would additionally allow differentiation between vaccinated and infected animals," the scientists wrote.
The AHS outbreak in Thailand has put Australian authorities on alert, given the possibility that infected midges could blow across waterways and gradually island-hop their way Down Under.
"There would be devastating consequences for the Australian equine industry if it were to establish here, due to the high morbidity and mortality in some strains," Dr. Mark Schipp, Australia's chief veterinary officer, said in an emailed response to questions from VIN News.
"Australia continues to monitor the outbreak of AHS in Thailand as part of our routine animal disease surveillance, and is engaging with other countries to develop a regional response to this outbreak."
Schipp said the main vector species behind the Thai outbreak, Culicoides imicola, is not in Australia. However, he said there are other Culicoides species in the country that might act as vectors for AHS. Wind movement of infected insect vectors, he confirmed, could spread the outbreak beyond Thai borders.
China's agricultural ministry said last week that it was taking samples from horses along its southern border with Thailand to check for AHS, according to a Reuters report.
Over land, midges tend to stay fairly local but can still travel up to a few kilometers per day by moving from host to host, according to Simon Carpenter, entomology group leader at the Pirbright Institute. The midges can travel even further if they enter wind currents higher in the atmosphere.
"Midges are fairly notorious for being able to fly long distances, mostly over water," Carpenter said. "Every now and again a midge-borne virus will pop up in an area where it hasn't been before and we can exclude animal movement as being the reason."
As for the chances of the Thailand outbreak reaching Australia, Carpenter said, "That's pretty unlikely, but it depends on how persistent the outbreak is. The AHS outbreak during the late '50s and early '60s that reached India shows how far this disease can travel if it's not knocked out relatively early by vaccination or doesn't burn itself out due to a lack of hosts."
Getting vaccines and protective netting right
The spread of AHS in Thailand is being managed, in part, by keeping midges away from individual animals, a tedious process that involves shutting them in stables protected by insect netting. Even the smallest gaps in stables need to be filled with silicone sealant to prevent the tiny insects from squeezing through. Netting and stables also are being sprayed with pyrethroid insecticide.
Insect netting 288

Photo by Dr. Siraya Chunekamrai
Insect netting with very fine mesh is required to protect horses from the biting midges — tiny, winged insects sometimes called gnats or no-see-ums — that transmit the virus that causes African horse sickness.
Chunekamrai said a challenge has been educating horse owners that ordinary mosquito netting isn't adequate. "The nets have to be finer than mosquito nets because the vectors are so small," she said. "If you use large netting, even proper netting, it creates an illusion that you are protecting the horse but you're not, really."
The disease so far has struck in eight of Thailand's 77 provinces, most heavily in the province of Nakhonratchasima, north of Bangkok, where the outbreak is thought to have originated. The first confirmed case was recorded on March 27 at a Bangkok laboratory by Thailand's Department of Livestock Development (DLD). On the same day, the OIE suspended Thailand's status as an AHS-free country, triggering import bans on horses from Thailand in countries around the world.
Containment efforts are complicated by the COVID-19 pandemic, which has infected at least 2,947 people in Thailand and killed at least 54, according to authorities. Thailand imposed a state of emergency on March 26 that forced the closure of many businesses and includes a 10 p.m.-to-4 a.m. curfew.
Practitioners fighting the AHS outbreak are taking the lockdown measures in stride, by the description of Dr. Metha Chanda, veterinary adviser for the Thailand Equestrian Federation. "It's affecting them, but not too much," he told VIN News by email. "The major problem is the curfew."
Chanda said volunteers are coordinating with government veterinarians employed by the DLD to target farms very early in the morning. "They are managing to finish the job and get home in time," he said. All veterinarians, Chanda added, are being encouraged to wear face masks and try to maintain a two-meter distance (a little more than six feet) from other people during the vaccination drive.
Chunekamrai, the veterinarian helping to lead the country's response, said it is too early to judge the success of efforts to quash the AHS outbreak. Containment efforts are targeting strategic locations, she said, including one close to the Cambodian border, to stop the virus from spreading deeper inside and outside of Thailand.
She said vaccines are not being administered to horses until after they have undergone polymerase chain reaction (PCR) and serology testing to ensure that only uninfected animals are vaccinated. In the meantime, horses are placed behind effective netting and microchipped so they can be easily identified later for vaccination.
Chunekamrai said horses can be given a low enough dose of live-attenuated vaccine to minimize the risk of midges potentially picking up the virus by biting a vaccinated horse. "So, if we're doing everything right, including having better protection, we should be able to mitigate all this," she said. "We are grateful to all the experts around the world who have generously shared their knowledge and resources with us, immediately and on an ongoing basis."
Chunekamrai, who also is vice president of the World Small Animal Veterinary Association, added: "Essentially, what we want is not just to control the disease now. We want our country-freedom status back. That is our goal."
Only a polyvalent vaccine — designed to treat multiple AHS serotypes at once — was immediately available to Thai authorities, despite only the AHSV-1 serotype being identified in the country. The vaccine currently being administered was donated by the company MaxWin and contains a mix of the AHSV serotypes 1, 3 and 4, a Thai government spokesperson confirmed. Chunekamrai said authorities have ordered and are still awaiting delivery of a second vaccine batch that uses only the AHSV-1 serotype.
Using a polyvalent vaccine carries the risk of establishing new disease serotypes in the population. There is also the possibility of gene segment reassortment occurring between outbreak and vaccine strains, potentially creating new genetic variants of the disease. An analysis by scientists from the University of Pretoria published in 2016 in the journal Infectious Emerging Diseases found that some AHS outbreaks in South Africa were caused by virulent revertants of AHSV type 1 live-attenuated vaccine, and reassortants with genome segments derived from vaccines containing AHSV types 1, 3 and 4.
"On one level, it's quite a difficult decision for them to use the current vaccine," Carpenter of the Pirbright Institute said. "But in terms of the damage the outbreak could do to everything else, using it now is a no-brainer. It's definitely the right thing to do."
Even if the outbreak in Thailand is contained swiftly, Carpenter said it already has provided a wake-up call to authorities globally about the risks posed by AHS. He noted that another pathogen spread by Culicoides, bluetongue disease, which affects ruminants, has appeared widely throughout Europe in recent years, highlighting the increased risk of AHS spreading due to global warming and globalization. Monitoring of wildlife shipments, including of zebras, may need to be tightened in the outbreak's wake, he added, while authorities everywhere also might want to consider stocking up on vaccines.
"The difficulty is that while we've got a lot of research on alternative vaccines, none of them have the market to be able to be used immediately in this situation," Carpenter said. "So there may be a requirement for things like vaccine banks to create a market for rapid development."